Actor Aishwarya Sakhuja, 41, a type 1 diabetic, recently shared a glimpse of the challenges that people with diabetes often face, especially at night. “When glucose levels won’t cooperate, neither does sleep. Continuous monitoring means continuous interruptions. This is what living with diabetes really looks like at night,” the Saas Bina Sasural actor expressed in a post on Instagram.
DISCLAIMER: This article is based on information from the public domain and/or the experts we spoke to. Always consult your health practitioner before starting any routine.
She also listed practices that help.
Balance your meals (don’t eat carbs alone)
Carbs spike sugar fast, but pairing them slows things down.
*Add protein (eggs, paneer, chicken, dal)
*Include healthy fats (nuts, seeds, ghee, avocado)
*Don’t skip fibre (vegetables, salads)
Be consistent with meal timing
Your body LOVES routine.
*Eat at similar times daily
*Avoid long gaps, as they can cause lows, rebound highs
*Late-night heavy meals = unstable overnight sugars (and CGM alarms)
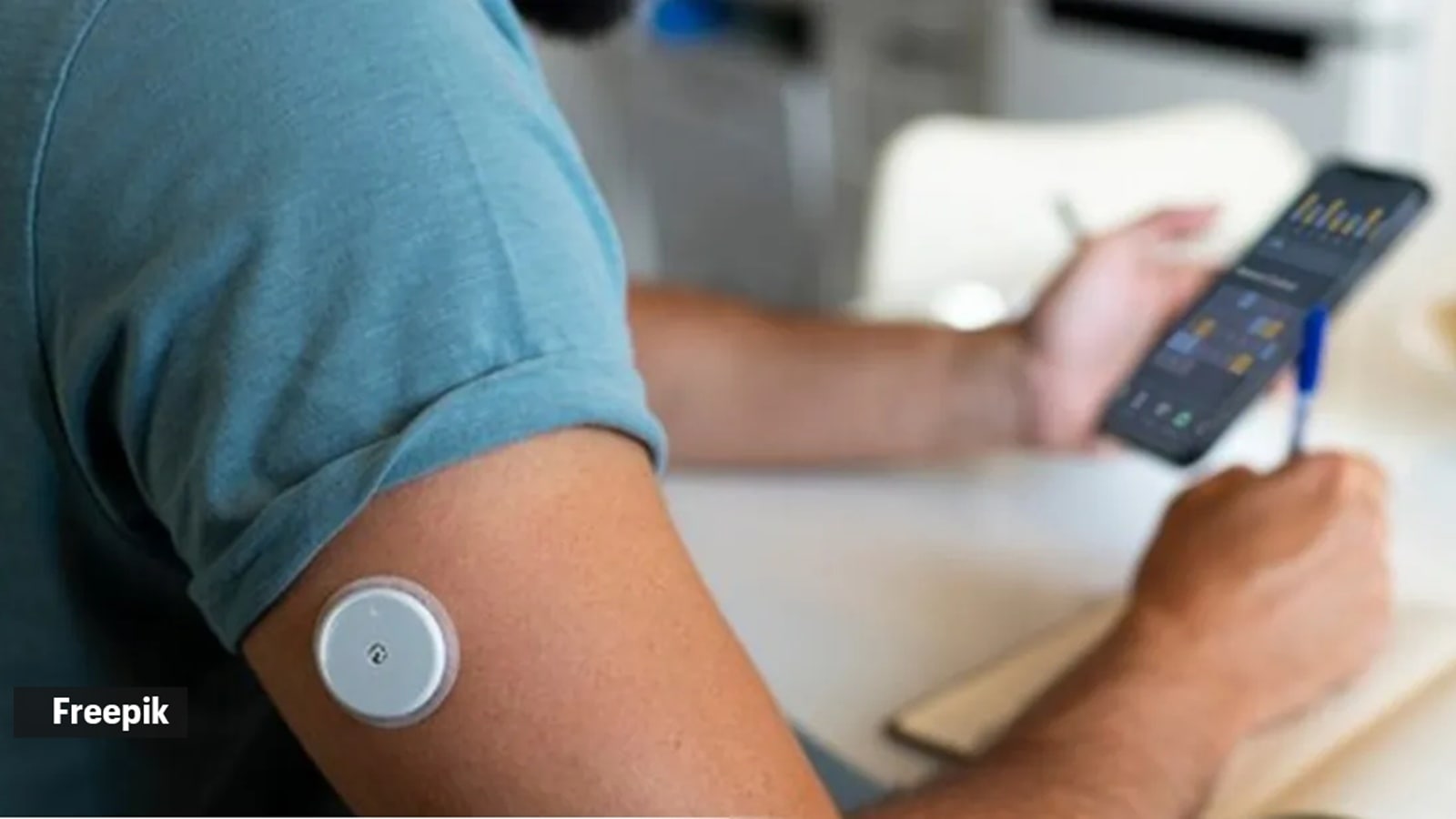 Are you tracking your sugar levels? (Photo: Freepik)
Are you tracking your sugar levels? (Photo: Freepik)
Move after meals
Even 10–15 minutes of walking after meals can:
*Reduce post-meal spikes
*Improve insulin sensitivity
This is one of the simplest and most powerful hacks, she said.
Watch high glycemic foods
Not all carbs behave the same.
Story continues below this ad
Try to limit:
*Sugary drinks, juices
*White bread, maida, sweets
Swap with:
*Whole grains (atta, brown rice)
*Millets, oats
*Low GI fruits (berries, apple)
Stay hydrated
Dehydration can mess with glucose levels.
*Aim for steady water intake throughout the day
*Helps kidneys flush excess glucose
Fix your sleep
Poor sleep = more insulin resistance + more unpredictable blood sugar.
*Try to sleep at consistent times
*Reduce late-night snacking
*Manage those CGM alerts with better pre-bed planning (like stable dinner + correct dosing)
Story continues below this ad
Taking a cue from her experience, we asked an expert about whether these practices help.
Dr Vijay Negalur, HOD – Diabetology at KIMS Hospitals, Thane, said sleep disruption in diabetes is more common than many realise. “Blood glucose levels don’t always follow a set pattern; they can drop too low or rise unexpectedly during the night. Both situations can cause symptoms like sweating, heart palpitations, or frequent urination, waking the person up. Additionally, while very useful, continuous glucose monitoring (CGM) devices can send alerts that interrupt sleep. Over time, these repeated disturbances impact sleep quality, which in turn worsens glucose control the next day,” said Dr Negalur.
What simple lifestyle measures can help stabilise glucose levels overnight?
A lot depends on what happens before bedtime. “The makeup of dinner is important; meals that mix carbohydrates with protein, healthy fats, and fibre lead to slower glucose absorption and fewer spikes. For example, instead of having carbs alone, pairing them with dal, paneer, or nuts can make a real difference. Keeping meal times consistent is also key; irregular eating patterns can confuse the body’s insulin response and cause fluctuations at night.”
Does physical activity after meals really help?
Yes, and it’s one of the most underrated tools. “Even a short 10 to 15-minute walk after dinner can improve insulin sensitivity and lower post-meal glucose spikes. This simple habit often leads to more stable readings overnight and fewer unexpected alarms,” said Dr Negalur.
Story continues below this ad
Are there specific foods people should avoid in the evening?
High glycaemic index foods, such as sugary drinks, refined flour products, and sweets, should be minimised, especially at night. “These cause rapid spikes followed by drops, which can be particularly disruptive during sleep. Choosing whole grains, millets, oats, and low glycaemic fruits like apples is a smarter choice,” said Dr Negalur.
How important is hydration and sleep routine in diabetes control?
Both are often overlooked but very important. “Dehydration can lead to higher glucose levels in the blood, while poor sleep increases insulin resistance. Sticking to a regular sleep schedule, avoiding heavy late-night meals, and planning dinner carefully can help reduce nighttime glucose swings. In many cases, better nights lead to better numbers the next day,” said Dr Negalur.




Leave a Reply